Gynecomastia
Conveniently located to serve the areas of Houston and Katy, TX

Gynecomastia is enlargement of normally occurring breast tissue in males that can affect one or both breasts. Men with gynecomastia are often self-conscious about their appearance and may try to hide their condition rather than pursue cosmetic surgical treatment for gynecomastia. Dr. Bonnor M.D, F.A.C.S. can evaluate and correct the appearance of gynecomastia into a more masculine aesthetically pleasing chest. Contact us or call (281) 579-5638 to explore your options.
Contents
About Gynecomastia
Gynecomastia occurs naturally at different times in a male’s life: at birth newborn boys are under the effect of estrogen from their mother and over half of newborn males will have gynecomastia that resolves in two to three weeks. Then at puberty while hormone levels are changing, gynecomastia can occur and usually resolves two years after the start of puberty. Then at midlife one in four males have some breast enlargement resulting from an imbalance of estrogen relative to testosterone. Other conditions that can cause gynecomastia include: obesity, lack of good nutrition, liver disease, anabolic steroids, estrogens, spironolactone, digoxin, finasteride. This list is not exhaustive but only to show that not only medical conditions but also some medications can cause gynecomastia.

Treatment Options
Gynecomastia Surgery
Due to the fact that gynecomastia is defined by overactivity of glandular breast tissue, oftentimes the condition can be treated by removing this breast tissue[1]. When indicated a surgical resection is performed by placing an incision at the skin-areola junction. In other cases, a liposuction procedure may be used to reduce stubborn fat in the chest associated with a mild gynecomastia.
Pseudogynecomastia Treatment
Diet and exercise are the ideal methods of maintaining a healthy physique. But even after significant weight loss, the body does not always conform to your ideal dimensions. Fat may persist in areas that you want slimmed down. Many men who experience massive weight loss complain that they still have too much volume in their chest. Enlarged male breasts that are not caused by glandular activity is a condition known as pseudogynecomastia[2].
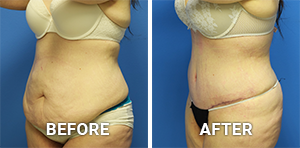
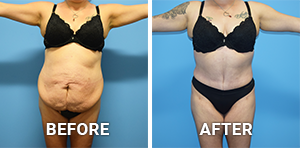
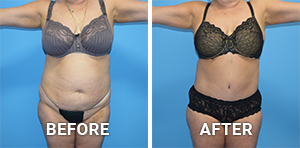
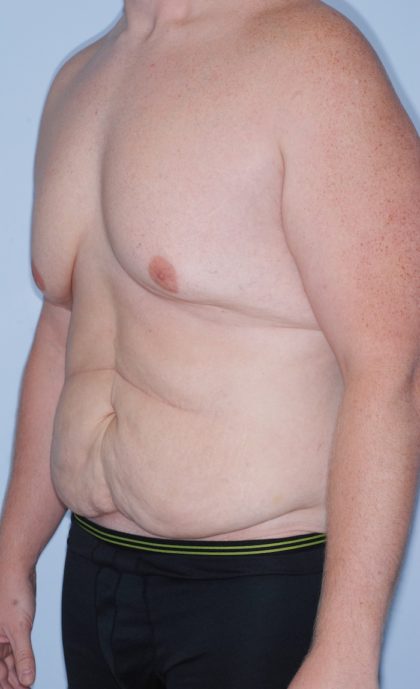
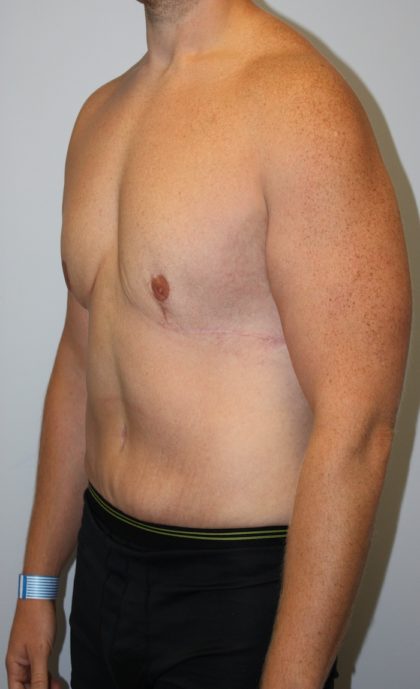
Before and After Photos
Procedure
Gynecomastia surgery is an outpatient surgery. Dr. Bonnor will schedule a follow-up appointment the next day to check your progress and replace any dressings of the treatment area. You may experience some minor bruising and swelling, but these effects should subside after the first week. Please avoid strenuous activity for four weeks, especially movements that place undue stress on your pectoral region.
Aftercare
Dr. Bonnor will discuss your aftercare protocols during your comprehensive consultation. These instructions will be tailored specifically to your case. Be sure to wear any compression garments to help your body heal and conform to its new shape. Your chest will be flatter and more aesthetically pleasing. Men who undergo gynecomastia surgery report increased confidence and an overall improvement in their quality of life[3].
Frequently Asked Questions (FAQ)
Am I a good candidate for gynecomastia surgery?
If you feel that you may be experiencing gynecomastia, then you may want to consider a visit to Texas Surgical Arts. To be an ideal candidate, you should be at or near your goal weight. During your consultation with Dr. Bonnor, please mention any existing health conditions that may prevent or postpone gynecomastia surgery.
What are the risks involved with gynecomastia treatment?
There are risks involved with any invasive procedure such as bleeding, blood clot, adverse reaction to anesthesia, or infection. Call (281) 579-5638 to schedule a consultation with Dr. Bonnor and discuss your concerns before proceeding with gynecomastia surgery.
What causes enlarged male breasts?
Many adolescent boys experience early signs of gynecomastia during puberty as a result of hormonal fluctuations. Some young men carry gynecomastia into adulthood. Male breasts can become enlarged later in life due to the reduction in testosterone production. Regardless of the root causes of gynecomastia, Texas Surgical Arts can address the persistence of enlarged breast tissue. Contact us to explore your options.
References
- Johnson, R. E., & Murad, M. H. (2009, November). Gynecomastia: pathophysiology, evaluation, and management. In Mayo Clinic Proceedings (Vol. 84, No. 11, pp. 1010-1015). Elsevier. https://doi.org/10.4065/84.11.1010
- Gusenoff, J. A., Coon, D., & Rubin, J. P. (2008). Pseudogynecomastia after massive weight loss: detectability of technique, patient satisfaction, and classification. Plastic and Reconstructive Surgery. 122 (5) 1301-1311. DOI: 10.1097/PRS.0b013e3181881df4
- Kasielska-Trojan, A., & Antoszewski, B. (2017). Gynecomastia surgery—impact on life quality: a prospective case-control study. Annals of Plastic Surgery. 78 (3) 264-268. DOI: 10.1097/SAP.0000000000000860